
Healthcare is one of the industries where the cost of late decisions is especially high. The examples are clinical deterioration, preventable readmissions, capacity shortages, and delayed interventions. They rarely occur unexpected. As care delivery becomes more complex and data-intensive. Healthcare organizations that rely on retrospective analysis cannot be reliable.
AI predictive analytics has become a response to this structural limitation. Modern healthcare departments can generate vast streams of clinical and behavioral data through electronic health records, diagnostic systems, connected devices, and administrative platforms. Yet without predictive models, this data can explain the past better.
When Ai is implemented with clinical relevance, data discipline, and workflow alignment. Predictive analytics supports safer care, more stable operations, and better use of limited resources, and this is where Acropolium comes in. As an expert healthcare development company, we help healthcare industry to shape predictive models. We make them aligned with real clinical workflows, regulatory constraints, and operational realities based on your real requirements.
What is AI predictive analytics in healthcare?
AI predictive analytics in healthcare applies machine learning technology and advanced statistical methods. It applies it for the collecting all clinical, operational, and behavioral data to forecast future events with practical relevance to care delivery. The focus is on estimating what is likely to occur next: patient deterioration, readmission risk, disease progression, demand surges, or operational strain, early enough to influence outcomes.
At its core, predictive analytics transforms healthcare data into forward-looking insight. Historical records and real-time signals are analyzed together to surface patterns that correlate with specific outcomes. Rather than producing definitive answers, models generate probabilities and risk levels that inform clinical judgment and operational planning. Predictive analytics is introduced to address specific clinical and operational challenges rather than to replace existing systems. Common objectives include:
Early identification of patients at elevated risk, enabling intervention before escalation;
Risk stratification that prioritizes attention and resources where impact is highest;
Personalization of treatment and follow-up based on observed response patterns;
Demand forecasting in healthcare and utilization to stabilize staffing, capacity, and supply planning.
Predictive analytics relies on models that learn from past outcomes and continuously adapt as new data is introduced. Statistical techniques establish baseline relationships, while machine learning methods refine predictions by recognizing non-linear patterns across large, heterogeneous datasets. As care protocols evolve and patient populations change, models are retrained to preserve accuracy and clinical relevance.
Healthcare environments generate data at different speeds and levels of structure. Predictive systems are designed to process structured clinical data alongside unstructured information such as free-text notes, imaging metadata, and device telemetry. This broader analytical surface allows models to account for nuance that traditional reporting tools cannot represent.
How does AI predictive analytics work in medical systems?
Predictive analytics AI converts fragmented clinical and operational data into forward-looking signals that support earlier and more informed decisions. Rather than replacing clinical judgment, predictive systems extend it by identifying patterns, risks, and trajectories that are difficult to detect through manual review or traditional reporting. The process unfolds through several tightly connected stages, each designed to preserve clinical relevance and operational usability. 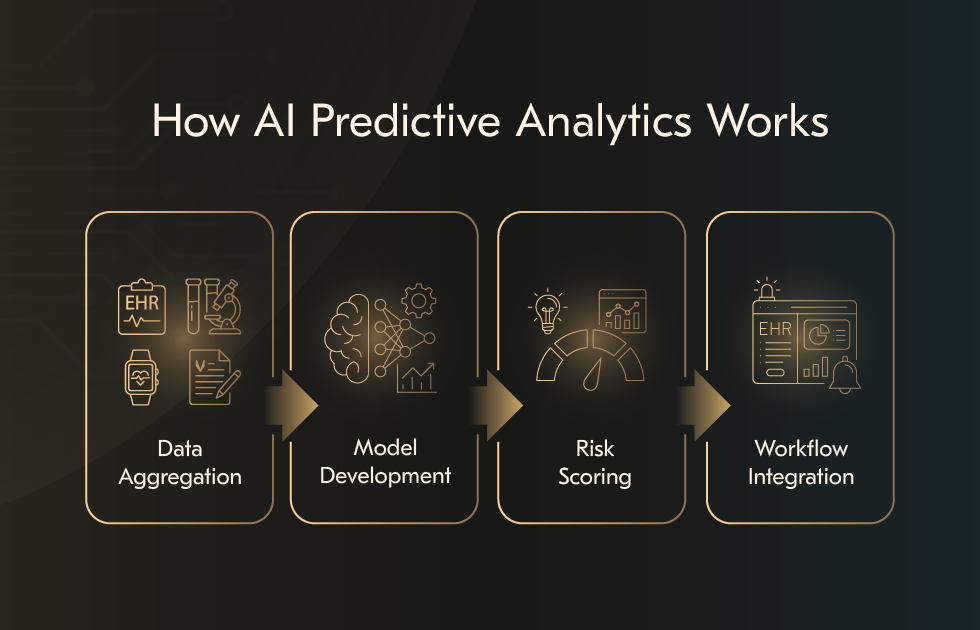
1. Data aggregation
Predictive analytics begins with consolidating data from across healthcare systems. Clinical records, laboratory results, imaging metadata, device telemetry, and administrative data are brought together into a unified analytical layer. Structured information includes all the diagnoses, medications, and vitals. Predictive analytics combined it with unstructured inputs, including physician notes and discharge summaries, using advanced language processing techniques.
In environments that rely on connected devices, real-time streams from wearables and IoT sensors add continuous physiological context. External factors can be not obvious during the assessment, such as demographics or social determinants of health. For them, it is better to incorporate to improve risk sensitivity and population-level insight.
2. Predictive model development
Once data is curated and validated, predictive models are trained using historical cases with known outcomes. AI model selection depends on the clinical or operational objective of the departments. This factors count on the predicting readmission risk, deterioration, or demand surges. During training, algorithms learn associations between patterns in the data and subsequent events. Unlike static statistical approaches, machine learning models adapt over time. As new data becomes available, it keeps predictions aligned with care practices and patient populations.
3. Risk scoring and forecast generation
After training, predictive analytics AI models evaluate current patient or operational data to estimate the probability of future events. Outputs typically take the form of risk scores or probability ranges rather than binary decisions. To support clinical usability, scores are often grouped into priority bands that indicate relative urgency. This approach enables early identification of patients who may require closer follow-up care, preventive intervention, or real-time health monitoring systems, as well as forecasts related to admissions, staffing demand, or equipment utilization.
4. Integration into clinical and operational workflows
Predictive insight can be helpful only accessible at the point of decision. Integration focuses on embedding predictions into EHR interfaces. Sometimes it is more than just the simple integration and it includes operational dashboards and care management platforms. Alerts and forecasts are designed to align with established workflows. Interoperability layers connect predictive engines with legacy infrastructure. The most important advantage is the continuity of data flow in the architecture. Human oversight remains central. You would ask why it still needed? Clinicians and administrators validate and act on predictive signals within defined governance boundaries.
What are the key benefits of predictive analytics in healthcare?
Predictive analytics matters in healthcare for several reasons. Many of the most costly and risky decisions are made under uncertainty. Clinical deterioration or preventable readmissions rarely occur without warning. The challenge lies in recognizing weak signals early enough to act on them.
Predictive analytics addresses this gap. The solution can turn existing clinical and operational data into actionable foresight, allowing healthcare organizations to intervene earlier, provide hospital resource optimization more accurately, and reduce avoidable risk at scale. For complex healthcare organizations, this capability directly affects the quality of care, financial stability, and long-term resilience.
Enhanced patient outcomes
Patient outcomes are shaped by clinical expertise and timing. AI in predictive analytics improves safety by identifying elevated risk before deterioration becomes visible in standard monitoring:
Earlier identification of chronic and acute conditions supports timely intervention and reduces avoidable complications;
Personalized treatment planning aligns therapies with individual risk profiles;
Continuous risk monitoring enables early warning systems in high-acuity settings;
Faster clinical response lowers mortality and serious adverse event rates.
Operational efficiency
Healthcare operations operate under constant pressure from fluctuating demand and limited infrastructure. McKinsey estimates that up to 40% of administrative activities in healthcare could be automated or augmented with AI. This research highlight the role of predictive analytics in reducing operational friction.
AI in healthcare introduces stability by replacing reactive adjustments with informed planning:
Forecasting admissions and discharges improves bed and capacity planning;
Staffing models associated with predicted demand reduce burnout and overtime costs;
Patient flow optimization lowers emergency department congestion;
Administrative automation reduces manual workload and process delays.
Cost reduction
Financial pressure in healthcare often stems from preventable events and more often from unavoidable care costs. AI predictive analytics helps control expenses. The major benefits of AI are reducing inefficiency and unnecessary utilization:
Targeted discharge planning lowers readmission rates and associated penalties;
Supply forecasting minimizes waste and stock shortages;
Predictive maintenance prevents equipment downtime and emergency repairs;
Early detection of billing anomalies limits revenue leakage.
Cost control achieved through prediction preserves care quality while improving budget reliability.
Population health analytics and preventive care management
Managing large patient populations requires episodic treatment and more technology innovation. Predictive analytics works on the anticipation trends and allocate resources where prevention has the real impact on health management:
Early detection of population-level risk patterns supports timely public health response;
Risk stratification focuses preventive programs on high-need groups;
Resource planning aligns community care services with projected demand;
Longitudinal monitoring improves outcomes across chronic disease cohorts.
Preventive focus reduces long-term care costs and improves system-wide health outcomes.
Benefits for health insurance
Payers face similar uncertainty in risk assessment and cost forecasting. Predictive healthcare operations analytics improves consistency across these functions:
Risk modeling supports fairer underwriting and coverage planning;
Claims processing becomes faster and more accurate;
Denial rates decline through earlier identification of high-risk claims;
Alignment between care outcomes and reimbursement improves financial transparency.
What are the real-world healthcare predictive analytics use cases?
AI predictive analysis delivers the most value in healthcare when it is applied to concrete operational and clinical problems. Predictive models help anticipate demand, detect risk earlier, and reduce avoidable inefficiencies across care delivery and administration. Below are representative use cases, each followed by a real implementation from Acropolium that illustrates how predictive analytics works in production healthcare systems.
Predictive resource planning
One of the use cases for predictive analytics in healthcare is operational healthcare data forecasting. Hospitals and care networks must continuously balance staff availability, equipment usage, and patient inflow, often under conditions of uncertainty. Predictive models analyze historical utilization, seasonal patterns, and near-real-time operational data to forecast workload, anticipate bottlenecks, and support more accurate resource allocation decisions.
In one of our projects, we built an AI-driven predictive analytics solution for healthcare resource planning. The system analyzed historical operational data. In this way, hospitals can forecast demand across facilities and departments, helping healthcare administrators plan staffing and capacity more effectively. Predictive AI-driven healthcare insights were embedded directly into planning workflows, supporting proactive decisions rather than retrospective adjustments.
Early risk detection
Predictive analytics is integral to early risk detection systems. This solution works only when combined with continuous data streams from connected medical devices. Real-time monitoring systems generate large volumes of physiological data that exceed human capacity for monitoring. Predictive models can identify subtle trends indicating deterioration long before clinical symptoms become obvious.
We implemented an IoT-based emergency health monitoring system for a leading healthcare company. Our team started with the assessment and used predictive analytics to analyze sensor data from connected devices to detect early warning signs. The platform supported continuous patient monitoring and generated alerts. This feature is especially useful when risk thresholds were approached. Our client gained the opportunity to respond faster clinically. Predictive models were designed to operate reliably in real time, where latency and data variability directly affect patient safety.
Predicting appointments in outpatient care
Outpatient clinics face persistent revenue loss and scheduling inefficiency due to appointment no-shows and late cancellations. Predictive analytics can identify behavioral patterns and contextual signals associated with missed appointments. Imagine when forecasts would allow clinics to intervene proactively through targeted reminders, dynamic scheduling, or overbooking strategies.
In a SaaS appointment scheduling platform for a medical clinic, we implemented predictive models to forecast appointment attendance. The system analyzed historical booking behavior, timing patterns. This way the patient engagement signals to estimate no-show probability. These insights helped clinics reduce idle capacity, stabilize daily schedules, and improve overall operational efficiency.
Patient risk prediction
Predictive analytics is increasingly used in patient- and clinician-facing apps. One of the context where it is used is the support longitudinal risk assessment. Such systems combine clinical history, ongoing monitoring data. Moreover, the behavioral indicators help to stratify patients by risk level and support personalized care pathways. Regulatory compliance and data security are central constraints in this healthcare use case.
We delivered a HIPAA-compliant medical application that incorporated predictive analytics for patient risk stratification and care monitoring. Predictive models operated within a secure architecture designed to meet healthcare privacy and compliance requirements.
How do predictive analytics vs traditional healthcare analytics differ?
Temporal orientation
Traditional healthcare analytics is designed to analyze historical data and explain past performance. Insights from it are typically reviewed after events have occurred. This data supports only reporting, auditing, and compliance.
AI and predictive analytics extend the decision horizon. Advanced technology output systematically estimates future risks and demand before issues escalate.
Reactive reporting vs proactive intervention
Conventional analytics supports reactive decision-making. Reports and dashboards highlight trends after outcomes are known. Healthcare predictive analytics enables proactive care for the patients. The mechanism of the applying AI works on the surfacing early warning signals, such as patient deterioration risk or admission surges.
Static analysis vs adaptive learning
Traditional analytics in healthcare is based on predefined metrics and fixed analytical logic. Predictive solution in 2026 applies machine learning technology models. What these models can do? They adapt as new data becomes available. This form of continuous learning enables forecasts and risk assessments to evolve. They improve always as patient populations as treatment protocols, and operational patterns change.
Data scope
Traditional healthcare analytics performs best with structured datasets. Artificial Intelligence predictive analytics incorporates different data even unstructured clinical documentation, device telemetry, imaging metadata, and longitudinal patient histories. This extended scope of AI and data functionality supports more nuanced risk assessment and pattern detection.
Actionability
Traditional analytics outputs are often consumed outside daily workflows through periodic reports. Predictive analytics embeds insights directly into clinical and operational systems, delivering risk scores, alerts, or forecasts at the point of decision. Actionability depends less on visualization and more on timing and contextual relevance.
| Dimension | Traditional healthcare analytics | Predictive analytics in healthcare |
|---|---|---|
| Time orientation | Retrospective analysis of past events | Forward-looking estimation of future outcomes |
| Primary questions answered | What happened and why | What is likely to happen next |
| Clinical impact | Indirect, often delayed | Direct support for early intervention |
| Data scope | Mostly structured historical data | Structured, unstructured, and real-time data |
| Insight delivery | Reports and dashboards | Embedded risk scores and forecasts |
| Model behavior | Static analytical logic | Continuously refined learning models |
| Operational use | Performance review and compliance | Proactive planning and decision support |
What are the real-world challenges of AI predictive analytics in healthcare?
AI predictive analytics can strengthen clinical and operational decision-making. Yet its adoption in healthcare remains uneven. The barriers are rarely isolated technical issues. Most failures occur when data, clinical practice, regulation, and organizational reality move at different speeds. Understanding these implementation challenges upfront is critical. 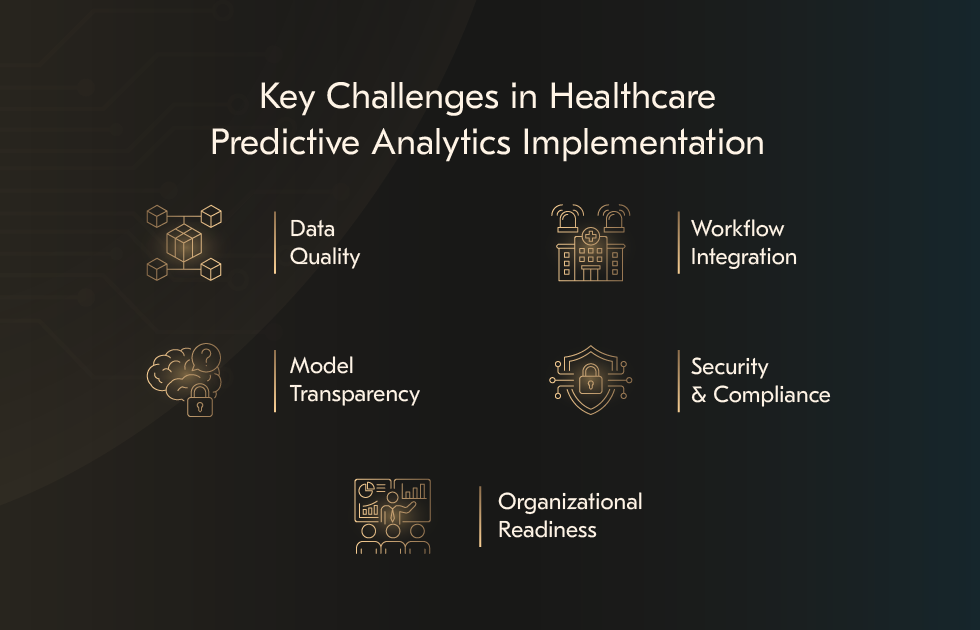
Data quality
Predictive models are only as reliable as the data they learn from. Healthcare data is often fragmented across many different EHR, laboratory systems, imaging platforms, billing tools, and external providers. Inconsistent coding standards, missing historical context, and delayed updates weaken model accuracy. Unstructured clinical documentation adds another layer of complexity. When data is unstructured, the AI can hallucinate more frequently. As physician notes and discharge summaries require careful processing before they can be used safely in predictive medical data modeling. Without disciplined data governance, predictive outputs risk contradicting clinical reality.
Model transparency
Many predictive models produce accurate forecasts without clearly explaining how they arrived at their conclusions. According to IBM, around 30% of healthcare executives entirely trust AI-generated insights. This stats highlights the importance of explainability, governance, and clinical oversight. It is one of the most important tricks for predictive analytics adoption.
Limited interpretability makes clinicians cautious. Those risks significantly impact the reputation of the company, particularly influence triage, treatment escalation, or discharge planning. Bias remains a parallel concern for everyone.
Models trained on narrow or imbalanced datasets may systematically misestimate risk for certain patient groups. Non reliable AI models can simply create ethical exposure and undermine confidence in analytics-driven recommendations.
Workflow integration
Another challenge may be not as obvious as others. But not all the teams think ahead the integration. It emerges when analytics tools sit outside established clinical and operational workflows. Legacy systems often restrict interoperability, while alert fatigue and poorly timed notifications reduce adoption.
Risk scores generated without clear ownership or follow-up responsibility;
Alerts that arrive too late or too frequently to support clinical action;
Predictive outputs that require manual reconciliation across systems;
Increased cognitive load for clinicians rather than decision support.
Without workflow alignment, predictive analytics and AI add complexity rather than reduce it.
Security exposure
Healthcare predictive analytics operates under strict regulatory oversight. HIPAA and GDPR regulations impose limits to each healthcare environment. It protects the patients on how data is collected, processed, and retained. Accountability remains legally ambiguous when algorithmic recommendations influence care decisions. Security concerns intensify as predictive platforms centralize sensitive clinical and operational data. Stakeholders must count on regulatory compliance to not be fined.
Organizational readiness
Predictive analytics is not a one-time deployment. Sustained value requires ongoing model monitoring, retraining, and governance as care patterns and patient populations change. Many organizations underestimate the operational effort needed to maintain predictive systems over time. But without the clear collaborate efforts the long term success may not happen. Overreliance on automated predictions without defined clinical oversight further increases risk. Long-term success of the idea depends on multidisciplinary collaboration, and a shared understanding of where algorithmic support ends and clinical judgment begins.
How Acropolium builds predictive analytics solutions for healthcare industry?
Acropolium approaches predictive analytics in healthcare as an engineering discipline. All our solutions are grounded in delivery experience and regulated-domain expertise. Over 22 years of software engineering work have established a delivery model for different size and industry businesses. In our values are the prioritization of clinical relevance, system reliability, and predictable execution over experimentation.
Predictive analytics initiatives start with a clear understanding of how healthcare organizations actually operate. Data sources, clinical workflows, regulatory constraints, and decision points are mapped before any AI predictive modeling work begins. We work to ensure that predictive insights support concrete actions, such as risk stratification, capacity planning, or care coordination.
Deep experience across healthcare, IoT, analytics, and SaaS
Healthcare predictive analytics often spans multiple technical domains. It could be a hospitals, laboratories, etc. We combine experience in healthcare software development, IoT data ingestion, big data platforms, and SaaS delivery to build systems that work end to end. Clinical data from EHRs, real-time signals from connected devices, and operational data from scheduling or billing systems are integrated into an analytical foundation.
Engineering predictability into analytics projects
Predictive analytics initiatives must align all timelines and operating costs under control. Acropolium applies structured planning to reduce uncertainty at each phase. The most important engineering capabilities are the processes with technology and data preparation in our teams. Model development, validation, and integration follow clear acceptance criteria, allowing healthcare organizations to scale analytics capabilities.
End-to-end responsibility from concept to deployment
Work typically spans the full lifecycle:
Planning and ideation focused on clinical and operational value;
Data architecture and integration across healthcare systems;
Predictive model development and validation;
Secure deployment into production environments;
Ongoing monitoring and refinement as data patterns evolve.
Our experience extends beyond individual projects. Over the years, the team has delivered 450 applications, supported 148 partners and customers, helped three startups grow into unicorns, and worked with Fortune 500 organizations. Long-term engagement remains a core indicator of delivery quality, with multiple client relationships spanning over 10 years.
When does your healthcare organization need predictive analytics?
Predictive analytics becomes necessary when clinical and operational decisions require forward-looking insight rather than retrospective reporting. The following situations typically indicate that predictive analytics should be introduced.
When patient risks are identified too late, complications, deterioration, or readmissions occur after discharge rather than being anticipated during care planning.
When hospital capacity planning relies on averages, it leads to recurring shortages of staff, beds, or equipment during demand spikes and underutilization during quieter periods.
When early signs of clinical deterioration are missed, especially in acute or chronic conditions, delayed intervention increases length of stay and adverse outcomes.
If the administrative workload continues to grow, with rising claim denials, slow prior authorizations, and scheduling inefficiencies affecting financial stability.
If value-based care models are adopted, they require accurate risk stratification, population-level monitoring, and outcome-driven resource allocation.
When chronic disease populations consume a disproportionate share of resources, and disease progression or non-adherence remains difficult to predict.
If appointment no-shows and late cancellations persist, it creates revenue leakage and disrupts clinical schedules.
When several of these conditions are present, predictive analytics supports earlier intervention, more stable operations, and better alignment between care delivery and available resources.
If these signals reflect your current challenges, Acropolium can help assess readiness, define priority predictive analytics in healthcare use cases, and design predictive analytics solutions aligned with healthcare workflows and compliance requirements. Contact us to discuss how predictive analytics can be applied to your healthcare data.









![ᐉ⭐ Blockchain in Healthcare: [6 Real Use Cases Included]](/img/articles/blockchain-technology-in-healthcare/img01.jpg)


![AI in Healthcare: Examples, Use Cases & Benefits [2025 Guide]](/img/articles/ai-in-healthcare-examples-use-cases-and-benefits/img01.jpg)
![Custom Hospital Management Software [2025 Guide]](/img/articles/hospital-management-software/img01.jpg)
![Doctor On-Demand App Development [2025 Guide]](/img/articles/doctor-on-demand-app-development/img01.jpg)