
Key Takeaways
- Healthcare software modernization is necessary when legacy systems compromise operational efficiency, data security, and regulatory compliance.
- Its benefits include improved interoperability, patient engagement, and adherence to current regulations.
- Modernization approaches help you replace, rebuild, rehost, refactor & rearchitect your solution.
With the rising need for telemedicine, remote care, and contactless patient/staff interactions, many healthcare providers face the need to replace or rearchitect the legacy healthcare software they use with modern cloud-based solutions.
What’s the actual situation today? About 40% of NHS hospitals in England use outdated medical equipment, including X-ray and MRI machines, that are over a decade old. If your EHR or other medical software is obsolete, you definitely have (or soon will) a hard time keeping it running.
All due to the lack of experts that know how to maintain legacy healthcare solutions, the increasingly growing costs of hardware upkeep (about £20m spent on aging equipment in the past three years in the UK), and the system’s inability to cope with increased workloads.
Given all that, there are only two realistic scenarios — you can either go for a healthcare IT legacy system support or rearchitect the software infrastructure. This article explores the pros and cons of both healthcare legacy system modernization approaches so that you can make an informed decision.
What Is a Legacy System in Healthcare?
Legacy systems in healthcare are outdated software or hardware still in use despite newer, more efficient alternatives.
Legacy systems pose several challenges, including poor interoperability with modern technologies, heightened security risks due to outdated software, and costly maintenance. They often lack essential features, creating data silos that hinder access to comprehensive patient information and delay decision-making.
Additionally, these systems may struggle to meet evolving regulatory standards, leading to HIPAA/HITECH or GDPR compliance risks and potentially impacting the quality of patient care.
Now, how can you tell if you’re running a healthcare legacy application? Look for the following clues:
- Lots of processes must be done manually
- The number of data formats your system works with is very small
- Some processes take very long to complete due to the poor integration of various system modules
- If it works, it works; if it doesn’t, you can’t tell why
- There are no error handling procedures
- You cannot guarantee the security of your patients’ and organization’s data
- Your system can’t run big data analytics
- Your IT department is a money sink in constant need of hardware replacements
Rebuilding vs. Maintaining a Healthcare Legacy System
Any software gets old with time, and you must either replace the outdated healthcare software or try to keep it running at all costs. There are some obvious benefits and downsides stemming from both decisions.
| Maintaining healthcare legacy systems | Replacing legacy healthcare systems | |
|---|---|---|
| Benefits | 1. Staff is already trained and familiar with the system. | 1. Continued operational headaches and inefficiencies. |
| 2. No immediate costs, as the system was fully paid off. | 2. High maintenance expenses and potential security vulnerabilities. | |
| 3. The system still serves its original purpose effectively. | 3. Difficult to add new features or adapt to modern needs. | |
| 4. No disruption to current operations. | 4. Maintenance can be complex due to outdated technology. | |
| 5. Established system that has been customized over time. | 5. Further customization is challenging and often requires specific code. | |
| Challenges | 1. Ability to choose a future-proof tech stack. | 1. Migration process may disrupt usual operations. |
| 2. Improved security and scalability through cloud solutions. | 2. Requires training staff to use new tools. | |
| 3. Easier to add new features and improve patient services. | 3. Potential for bugs and issues that need to be resolved post-launch. | |
| 4. Centralized Electronic Health Records (EHR) system. | 4. Initial high costs for development and migration. | |
| 5. Reduces long-term liabilities and operational risks. | 5. Requires thoughtful planning and careful implementation. |
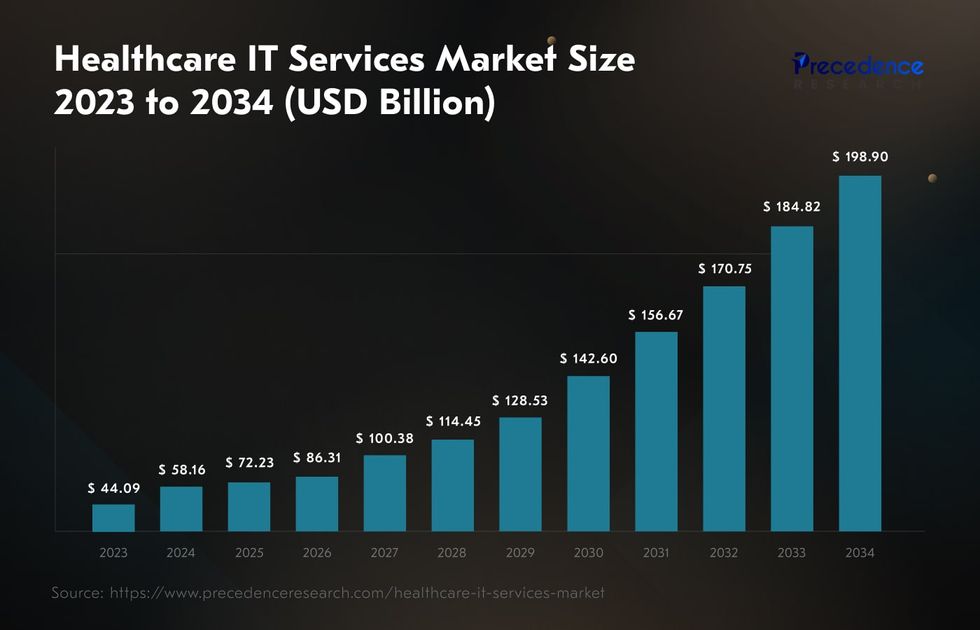
Whichever path you choose, this will never be the final decision, as you will have to rebuild the legacy healthcare system at some point in the future anyway, even despite the challenges it will bring. Given this, it’s unsurprising that the global healthcare IT services market is projected to grow from $58 billion in 2024 to $199 billion by 2034, with a CAGR of 11%.
Healthcare Legacy System Modernization Approaches
Naturally, there is no one-size-fits-all solution for healthcare legacy application modernization. But there are four main approaches to doing it: replacement, rebuilding, refactoring, and rehosting. Let’s take a closer look at each of them.
Replace
There are lots of SaaS products built for healthcare providers. You may find a solution that meets your core needs, and if certain features are missing, the vendor can develop them or offer plugins.
Replacing legacy systems with modern solutions enhances patient care by providing access to advanced functionalities and better data management. While this approach requires significant upfront investment, it leads to long-term operational efficiency.
Rebuild
If your system runs on incredibly old code like COBOL or FORTRAN, you can list the necessary functions and order them rebuilt from scratch using a modern programming language.
Rebuilding legacy systems lets you customize them according to the specific patient needs, improving the treatment quality. However, this requires significant development time and resources, which can disrupt operations during the transition.
Rehost
Sometimes the core of your system is too complex and fragile to be quickly replaced or rebuilt but is too resource-demanding to ensure the needed scalability and operational resilience. In that case, your systems move to cloud IaaS solutions, running on virtual machines and Docker containers instead of rack servers.
Rehosting legacy systems in a cloud environment offers quick access to data, enhancing patient care delivery with minimal initial disruption. While it simplifies infrastructure, it may not resolve existing system limitations, leading to future operational challenges.
Refactor & Rearchitect
Sometimes, your system uses an outdated programming language version, limiting backend logic and preventing updates. In that case, your technology provider must refactor the code to reimplement functionality using the latest stable versions of the programming language, databases, frameworks, and libraries. The same goes for rearchitecting the infrastructure.
Refactoring and rearchitecting legacy systems enhance SaaS scalability and performance, improving patient care through better service delivery and modern technology integration. Streamlining operations and reducing long-term maintenance costs, this approach demands significant investments.
As you can see, there are multiple approaches for healthcare legacy software modernization, so your organization can select the one that fits your business strategy and budget best.
Steps to Modernize Healthcare IT Systems
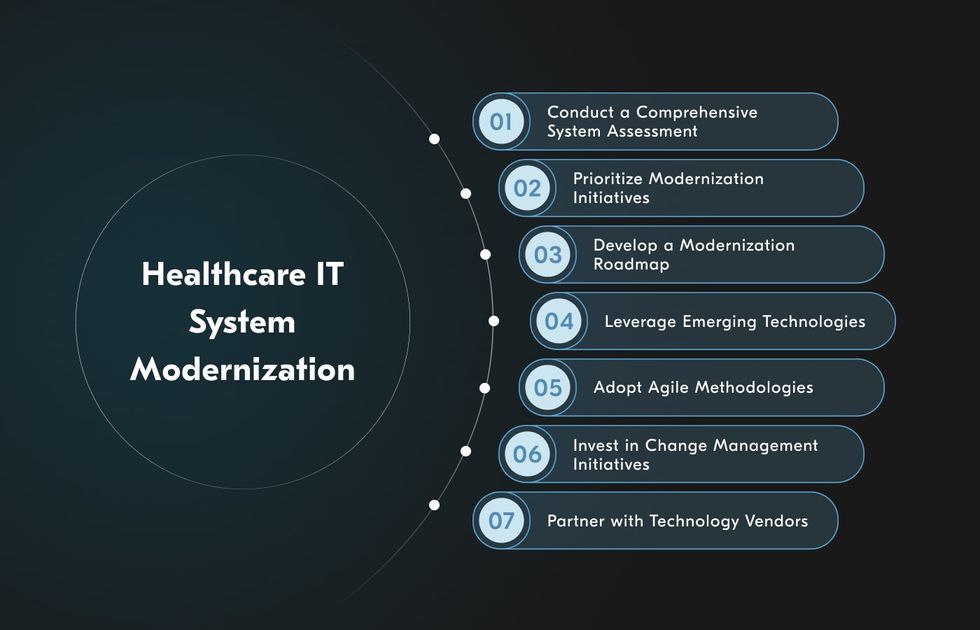
Here are the essential steps to modernize healthcare IT systems and stay ahead in the digital transformation journey.
1. Conduct a Comprehensive System Assessment
Begin by evaluating your current IT systems to determine their readiness for modernization. Test software and network performance and analyze security, compliance, and the overall technology stack. Identify areas of technical debt, inefficiencies, and risks associated with maintaining legacy systems.
2. Prioritize Innovation Initiatives
After assessing existing systems, prioritize modernization initiatives based on their potential impact on patient care and operational efficiency. Consider costs, regulatory requirements, system complexity, and stakeholder interests. Engage key stakeholders in discussions to ensure alignment and support for prioritized initiatives.
3. Develop a Modernization Roadmap
Create a comprehensive roadmap that outlines clear objectives, milestones, and timelines for each transformation initiative. Define specific goals, such as transitioning to cloud infrastructure or improving data security.
4. Leverage Emerging Technologies
Explore the integration of emerging technologies like cloud computing, artificial intelligence (AI), machine learning (ML), and the Internet of Things (IoT) into your healthcare systems. Cloud solutions ensure scalability, while AI and ML boost decision-making and patient outcomes. IoT devices enable remote monitoring and real-time data sharing.
5. Adopt Agile Methodologies
Implement Agile methodologies, such as Scrum or Kanban, to facilitate iterative development and deployment of modernization initiatives. By dividing the roadmap into smaller, manageable sprints, teams can focus on delivering specific features or improvements in short cycles.
6. Invest in Change Management Initiatives
Invest in comprehensive training programs to help IT staff and end-users become familiar with new technologies and processes. Change management initiatives are essential for demonstrating the benefits of modernization, highlighting how new systems will improve workflows and productivity.
7. Partner with Technology Vendors
Establish strategic partnerships with healthcare IT outsourcing experts to leverage their specialized knowledge and experience. Collaborating with vendors can provide valuable insights into best practices and innovative solutions tailored to your organization’s needs.
Healthcare Legacy System Modernization Cases
Companies across the industry successfully navigate the complex process, proving that legacy systems can be transformed into powerful, efficient digital ecosystems.
1. Mayo Clinic has successfully replaced Cerner and GE solutions with its $1.5 billion SaaS — Epic electronic health record (EHR) system. The project was complex, as it spanned multiple specialties and locations in Florida, Arizona, and Minnesota.
It was also difficult to manage the transition for a large and diverse workforce, which was addressed through a comprehensive change management strategy. As a result, patient care has been improved through simplified access to clinical and billing information, regardless of location.
2. The Cleveland Clinic EHR upgrade aimed to standardize and modernize clinical technology in more than 210 outpatient facilities and 18 hospitals worldwide. A key outcome was providing consistent, high-quality care across multiple locations, improving caregiver efficiency, and supporting global expansion.
Challenges included integrating legacy systems, aligning tools across specialties, and managing change for 66,000 caregivers. For example, outdated anesthesia systems required replacement with integrated modules. Clinician feedback was key to customizing tools and ensuring a smoother transition.
3. NHS trusts are actively modernizing their systems by decommissioning legacy platforms and migrating data to cloud-based solutions. This approach ensures efficient access to historical data, reduces costs, and enhances cybersecurity.
Key challenges include protecting patient data during system transitions, addressing cybersecurity risks, and managing high expenses. The operational demands of digital transformation also often conflict with the day-to-day functions of NHS organizations, causing delays and complications.
Why Choose Acropolium for Healthcare Legacy System Modernization?
Acropolium has 11+ years of experience in delivering healthcare app development services building new apps from scratch and upgrading existing solutions with modern web app architecture or tech stack. Be sure that we follow the latest healthcare trends, enriching projects with artificial intelligence and machine learning.
While most healthcare-related modernization cases are NDA-protected, we did find pharma and EHR examples to showcase the benefits of replacing legacy healthcare software with cloud-based tools.
AI-Based Pharma Application Development
A prominent healthcare provider partnered with Acropolium to develop a pharmaceutical app using AI to enhance patient engagement and streamline operations. We incorporated machine learning algorithms for improved prescription accuracy, automated inventory management, and in-app appointment scheduling.
Key outcomes included a 30% increase in efficiency through automated processes, a 15% growth in customer retention from personalized features, and a 25% reduction in data breach risks.

Blockchain-Based EHR Software Development
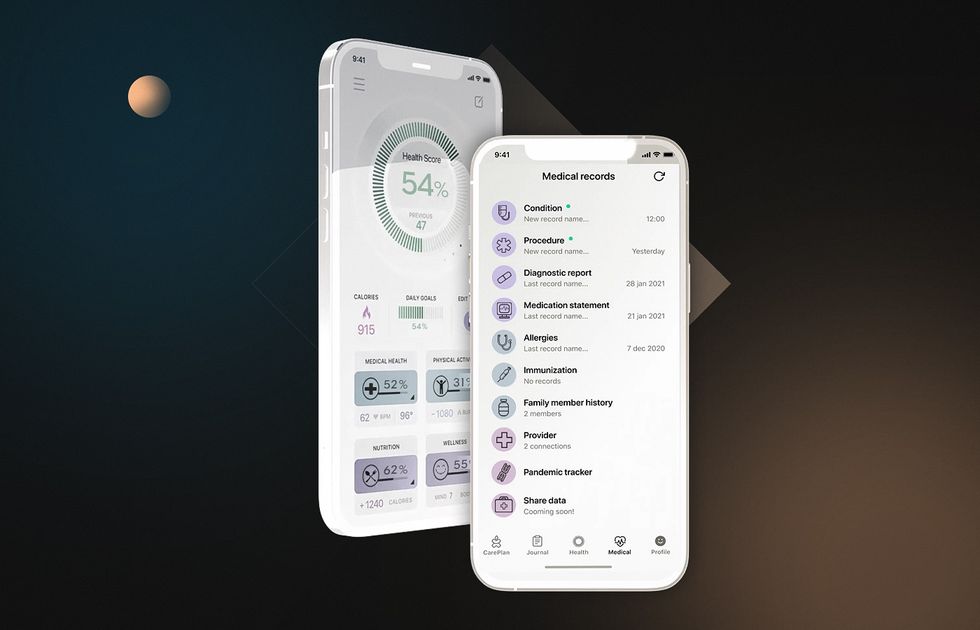
Let’s look at another legacy healthcare system example. A healthcare organization partnered with us to develop advanced EMR software and improve patient care. The project focused on creating an intuitive user interface to facilitate adoption and seamless integration with existing healthcare systems to eliminate data backlog.
The blockchain-based EHR solution was delivered on time. It seamlessly integrated with current healthcare systems and also increased user satisfaction with better.
Final Thoughts
Modernizing legacy systems is crucial for healthcare organizations. By transitioning to advanced, integrated solutions, the company can overcome data silos, reduce errors, and leverage innovative technologies like AI and blockchain. This transformation boosts patient engagement and satisfaction and helps medical providers adapt to the fast-paced changes.
We will be glad to assist you in updating your legacy healthcare system and selecting the most cost-efficient approach to meet your business goals. If you have questions about pricing models or want to discuss your subscription-based project, get in touch with Acropolium’s dedicated team, and let’s talk business!








![Custom Hospital Management Software [2025 Guide]](/img/articles/hospital-management-software/img01.jpg)
![Big Data in Healthcare: [Use Cases & Applications for 2025]](/img/articles/big-data-in-healthcare/img01.jpg)


![Cloud Computing in Healthcare [6 Real Use Cases Included] | Acropolium](/img/articles/cloud-computing-healthcare/img01.jpg)